HIPAA-Compliant Cleaning: What It Means and What It Doesn’t
Learn what HIPAA-compliant cleaning really means for medical offices and clinics, including vendor access rules, privacy safeguards, incident protocols, and what to require.

HIPAA-Compliant Cleaning: What It Means and What It Doesn’t
If you manage a medical office, clinic, or outpatient facility, you’ve probably heard the phrase “HIPAA-compliant cleaning.”
But that can just be a marketing buzzword if you don’t look a little deeper.
This quick guide helps you understand what HIPPA-compliant cleaning should actually entail, how it reduces avoidable privacy risk, and what needs to be defined with a vendor before work starts.
Before we go on, it goes without saying but this article isn’t legal advice. It’s just meant to give you a solid primer for your janitorial decision making.
That said, let’s answer the main question:
What is HIPAA-Compliant Cleaning?
HIPAA-compliant cleaning usually means a vendor is trained to work in healthcare spaces where protected health information may be present, follows access rules, and knows how to avoid unnecessary exposure to patient information. HHS says HIPAA applies to covered entities and business associates, and covered entities are expected to use reasonable safeguards and limit unnecessary access to protected health information.
What HIPAA has to do with cleaning vendors
This is where a lot of the confusion starts.
The issue is usually not with “medical cleaning” by itself. The issue is whether a vendor may come into contact with protected health information while doing normal work.
That can happen in 100 ordinary ways. A cleaner walks into an exam room and sees paperwork on a counter. They empty trash near a front desk. They clean near a printed schedule, specimen label, or a screen left visible after hours.
HHS says the HIPAA Rules apply to covered entities and business associates. But a cleaning vendor is not automatically treated as a business associate just because they work inside a healthcare building.
So let’s go a little deeper.
What “HIPAA-compliant cleaning” usually means in practice
For most facilities, this phrase should point to disciplined habits, not legal theater.
The goal is simple: reduce unnecessary exposure to patient information while keeping the site clean and running smoothly.
In practical terms, a healthcare cleaning vendor should have site-specific rules for access, after-hours entry, restricted areas, and incident reporting. Staff should know what to do if they come across visible patient information and when to stop, escalate, and notify the client.
That approach lines up with HHS guidance that covered entities should use reasonable safeguards and limit access to the minimum necessary for the job at hand.
A solid program usually includes:
- Staff training on privacy awareness in healthcare settings
- Clear boundaries around records areas, desks, screens, labels, and bins
- Role-based access to rooms and zones
- Site-specific instructions for keys, badges, alarms, and after-hours entry
- A documented escalation process if sensitive information is left exposed
- Supervisor oversight and routine check-ins
None of that is flashy. But this is the kind of operational discipline that makes a cleaning program feel safe to a practice manager.
What it does not mean
This is where buyers can get tripped up. A vendor can use the phrase confidently and still leave major gaps in scope, training, or access control.
For example, the phrase does not automatically tell you whether the vendor is a business associate under HIPAA. It also does not replace the facility’s own privacy policies, room controls, or staff responsibilities.
HHS makes clear that HIPAA status depends on whether an organization is a covered entity or business associate under the rule, not on a marketing label.
Instead of asking, “Do you call your service HIPAA-compliant?” the better question is, “What do your cleaners do to reduce avoidable privacy risk on my site?”
Are janitorial companies business associates under HIPAA?
This is one of the most important questions to look at, and the answer is usually more straightforward than people expect.
For ordinary janitorial work, the answer is generally no.
HHS says a business associate contract is not required for organizations whose services do not involve the use or disclosure of protected health information and where any access to PHI would be incidental, if at all. HHS specifically says janitorial services generally are not business associates because any disclosure that may happen during ordinary duties is limited and incidental.
But this can change depending on scope.
HHS also says the analysis changes when the service routinely involves PHI, such as handling records or shredding documents that contain protected health information. In that kind of situation, the vendor is much closer to business-associate territory unless the service is treated as part of the covered entity’s workforce under direct control.
That distinction matters because many facilities assume every healthcare vendor needs the same paperwork. In reality, the scope of work drives the privacy analysis.
What a medical facility should require from a cleaning vendor
This is where a smart buyer shifts from labels to specifics.
Whether you need hospital cleaning, outpatient clinic janitorial services, or cleaning for a medical offiice building or any other healthcare facility, good healthcare cleaning scope should make privacy expectations boringly clear.
At a minimum, require:
- A written scope of work by area
- Restricted-area rules
- After-hours entry procedures
- Clear boundaries around paper records, labels, screens, and bins
- A documented incident reporting process
- Site-specific staff training
- Supervisor oversight
- A single point of contact for questions and escalations
HHS says covered entities should use reasonable safeguards and policies that limit access to protected health information based on job responsibilities. So even when janitorial services don’t qualify as business associate entities, the facility should still expect disciplined, privacy-aware behavior.
Common risk points during cleaning
The biggest privacy problems are rarely dramatic. They’re usually small moments that are relatively easy to prevent.
Common examples include sign-in sheets left at the front desk, printed schedules on counters, visible labels on containers, unlocked offices, open file drawers, and computer screens left active after staff leave for the day.
Trash and disposal areas deserve attention too. HHS says covered entities must apply appropriate administrative, technical, and physical safeguards to protect PHI in any form, including in connection with disposal.
That means the facility and the vendor should be crystal clear about what belongs in normal trash, what belongs in shredding or secured disposal, and what staff must secure before cleaning begins.
Documentation that helps protect the facility
Good documentation doesn’t just support quality. It makes expectations visible before something goes wrong.
A healthcare cleaning program should have site-specific SOPs, training records, supervisor checklists, and incident logs. If access is controlled by keys, badges, or alarm codes, the facility should also know who has access and when. HHS guidance consistently points back to reasonable safeguards, workforce controls, and policies that limit unnecessary access to PHI.
This is also where stronger vendors separate themselves. Anyone can promise discretion. Fewer vendors can show you how that promise works on a Tuesday night when one cleaner is covering three suites and the last provider left in a hurry.
Questions to ask a cleaning vendor about HIPAA-related risk
These questions make vendor conversations much more useful. They help you move past vague assurances and into real operating detail.
Ask:
- How do you train staff to work around patient information?
- What should your cleaners do if they find PHI left out in the open?
- Which rooms or areas do you treat as restricted?
- How do you control after-hours access?
- Do you ever handle records, shredding, or other PHI-related tasks?
- What incidents do you document, and who gets notified?
- How do you supervise work in sensitive areas?
A strong vendor should be able to answer these clearly without overpromising. That is usually a good sign that the program is mature.
The bottom line
HIPAA-compliant cleaning is best understood as a set of privacy-aware healthcare cleaning practices, not a magic label.
Any janitorial service can adopt that phrase. So it’s important to make sure they actually have clear procedures, limited access, disciplined staff, and a realistic escalation process.
HHS guidance supports that practical view by focusing on covered-entity obligations, reasonable safeguards, and the difference between incidental exposure and work that routinely involves PHI.
If you are evaluating healthcare cleaning vendors, ask for the scope, the access rules, the training approach, and the incident process.
That is where the real answer lives.
If you want to pressure-test your current setup, request a site walk and review the scope room by room.
FAQ
What is HIPAA-compliant cleaning?
In plain English, it means a cleaning program designed to reduce avoidable privacy risk in a healthcare setting. That usually includes staff training, controlled access, and clear steps for handling incidental exposure to patient information. (HHS.gov)
Are janitorial companies covered by HIPAA?
Usually not. HHS says HIPAA applies to covered entities and business associates, and ordinary janitorial services generally are not business associates when any access to PHI is only incidental. (HHS.gov)
Is a cleaning company a business associate under HIPAA?
Generally not for ordinary janitorial work. HHS says the answer can change if the work routinely involves PHI, such as handling records or shredding documents with protected health information. (HHS.gov)
Does a cleaning company need a BAA?
Not usually for standard janitorial services where any PHI exposure is incidental. The analysis changes when the scope of work routinely involves PHI. (HHS.gov)
What should a healthcare facility require from a cleaning vendor?
Require a written scope, restricted-area rules, after-hours access procedures, privacy-aware training, and a documented incident process. That approach reflects HHS guidance around reasonable safeguards and limiting unnecessary access. (HHS.gov)
Is this legal advice?
No. This article is a practical guide for evaluating healthcare cleaning vendors. For legal interpretation of your specific HIPAA obligations, the facility should consult qualified counsel.
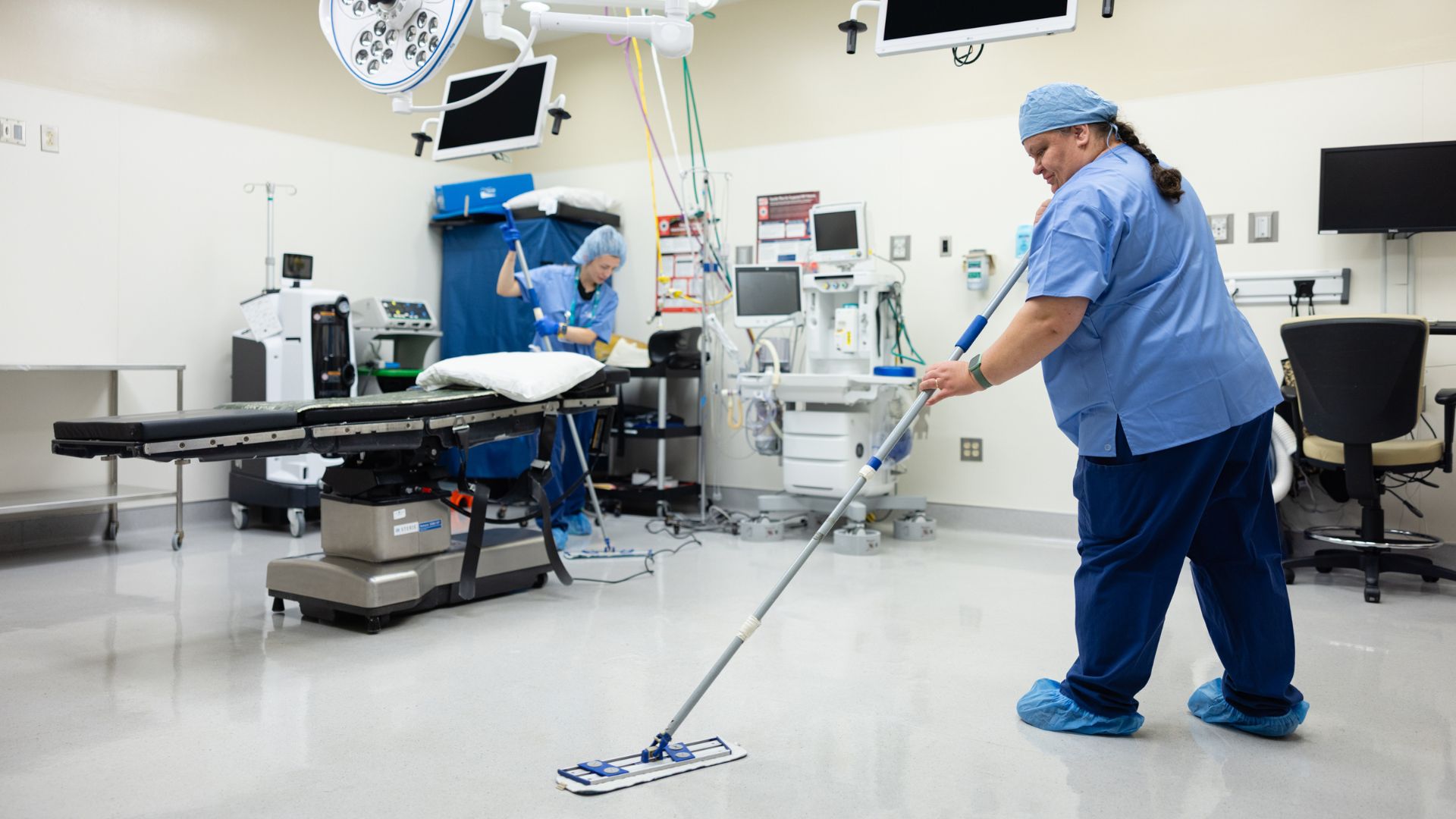
Learn what terminal cleaning means in healthcare, when it is needed, what it includes, and what to require from a medical cleaning vendor.
Read More
Learn what audit-ready healthcare cleaning documentation should include, from schedules and SOPs to training records, QA logs, and corrective actions.
Read More
Learn what HIPAA-compliant cleaning really means for medical offices and clinics, including vendor access rules, privacy safeguards, incident protocols, and what to require.
Read More
Hiring medical office cleaning services in Seattle? Use this checklist for scope, high-touch disinfection, turnover handoffs, logs, and QA. Request a site walk.
Read More
Best practices for clinic cleaning services: high-touch priorities, waiting rooms, restrooms, shared equipment boundaries, and checklists. Request a site walk.
Read More
Hospital janitorial services explained: what EVS covers, what to outsource, scope boundaries, and inspection-ready documentation. Request a walkthrough.
Read More


